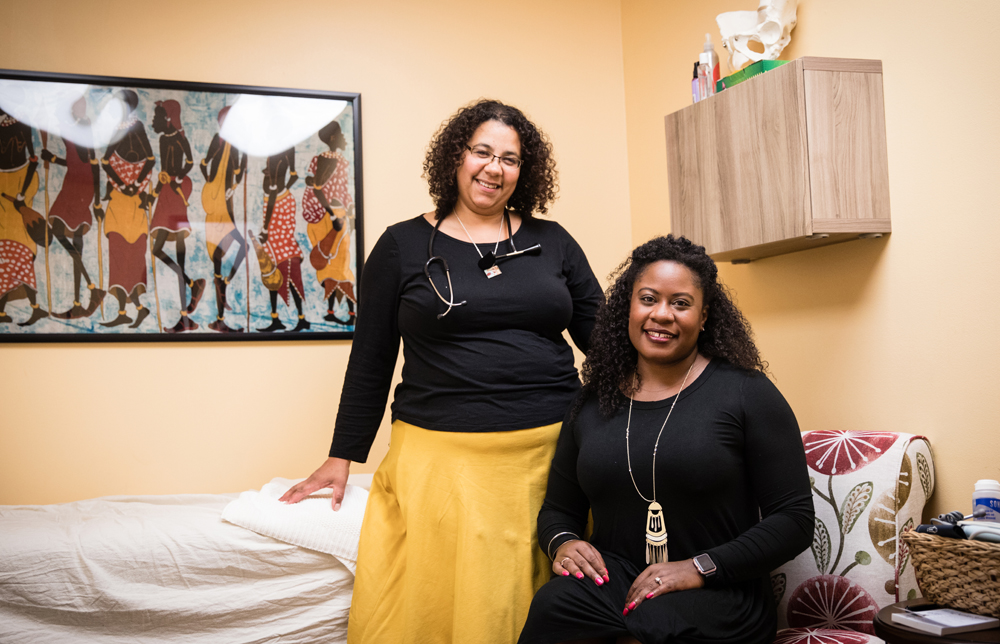“The persistent health inequities in our society stifle the opportunity of many to contribute fully to the future of our nation,” says Rachel Hardeman, a health equity researcher and assistant professor at the School of Public Health. “Racism has a detrimental impact on individuals and communities.”
The goal of Hardeman’s work as a public health professor is ambitious — to connect structural racism to health, to bring awareness to the issue, and to identify opportunities to dismantle structural racism and the systems and institutions that allow health inequities to persist.
Embedded in the Community
Hardeman’s interest in public health came while studying in Havana, Cuba. There, she saw a unique model for primary and preventive care where primary care physicians live where they work — their home is typically above the clinic. “There is a sense of responsibility and a relationship, a bond between doctor and patient that was unlike any I had ever seen before,” she says. “I immediately wondered, if we in the US were capable of offering this level of commitment and quality of care to all communities.”
One place Hardeman sees this model play out is at the Roots Community Birth Center in North Minneapolis, a community where nearly 50 percent of the population is African American.
Roots is the brainchild of Rebecca Polston, a practicing certified professional midwife (CPM) who wanted to make out-of-hospital births more accessible and more community focused. Her center is the only African American-owned birth center in Minnesota and one of only five African American-owned birth centers in the US. “Roots Birth Center is unique in that it’s embedded in one of communities in Minnesota that experiences the most unequal birth outcomes,” says Hardeman.

Those birth outcomes are staggering. African American women are four times more likely to die during childbirth than white women, according to the CDC. And in Minnesota, African American babies are twice as likely to die in their first year of life in comparison to white babies. Death statistics aside, Hardeman says African American women generally experience poorer quality of care and discriminatory treatment within traditional medical systems. “To know that not everyone has the opportunity for respectful care during their pregnancy and childbirth is really painful,” she says.
As a graduate student, Hardeman worked with maternal health policy researcher and Associate Professor Katy Kozhimannil on research which determined that birth doulas — professionals who support mothers before, during, and immediately after childbirth — improve birth outcomes for low income women and women from racial and ethnic minority backgrounds. Polston, aware of this work, approached Hardeman and Kozhimannil to discuss the potential for future collaborations.
In 2015, the three of them got their chance to bring a research perspective to Polston’s work through the Robert Wood Johnson Foundation’s Interdisciplinary Research Leaders (IRL), a program that brings together researchers and community members. “Rebecca came to us, and when people and communities outside of academia drive the idea, it ensures that what we’re doing will have an impact and will help people,” says Hardeman.
Through the IRL, Hardeman partnered with Polston and Kozhimannil to investigate the ways that community-connected and culturally centered clinical and support services can disrupt the well-worn pathways between social determinants of health and birth outcomes that have produced disparities for African American mothers and babies for more than a century.
Starting with Medical Schools
Our health is not solely a result of our biology, but depends in large part on our access to social and economic opportunities; the resources and supports available in our homes, neighborhoods, and communities; the quality of our schooling; and the cleanliness of our air, food, and water. Structural racism, the kind that is so ingrained in our society that we may not be aware of it, is a major health determinant.
Traditionally, future physicians receive very little training about how social determinants have an impact on the communities they will serve. Additionally, they are mostly unaware of the structual racism inherent in their own education.
Hardeman is determined to tackle both issues by targeting the education medical students receive. “This is where public health and medicine can really work together,” says Hardeman. “Public health provides the context to guide education on the social determinants of health.”
A main focus of Hardeman’s research is what’s called the “hidden curriculum” — unofficial and often unintended lessons that students learn in school. Ultimately, she’s identifying how medical institutions help systemic and structural issues — including racism — to persist. “Understanding how the hidden curriculum contributes to a medical student’s, and, ultimately, a physician’s understanding of health disparities and empathy can help transform our medical education systems and core values to better care for all populations,” says Hardeman.
To further understand this, Hardeman is a co-investigator on a research study called CHANGES (Cognitive Habits and Growth Evaluation Study). The study began in 2010 and surveyed a cohort of just under 5,000 first-year medical students from 50 medical schools around the country. The study is collecting data that focuses on implicit bias and attitudes toward empathy, as well as information about the students’ perceptions about diversity climates in their schools.
CHANGES has produced evidence that is making medical schools think twice about the training they provide — findings such as 64 percent of students report exposure to a negative racial climate at their school; 81 percent report witnessing discrimination; and 94 percent report negative role modeling. The study has also identified that a “negative diversity climate” places minority students, and all students, at a greater risk for depression. “When something negative exists, we all suffer because of it,” says Hardeman. “Fixing it will help both the students who feel it most and everyone in general.”
Speaking Out
The topic of Hardeman’s research — racism — is often a topic that people are uncomfortable discussing. Hardeman, however, hasn’t been afraid to have those uncomfortable conversations to raise awareness.
On the heels of Philando Castile’s 2016 death in Minneapolis, Hardeman, along with collaborators Kozhimannil and Dr. Eduardo Medina of Park Nicollet Clinics, published an editorial in the New England Journal of Medicine that identified five ways clinicians and researchers can dismantle structural racism and support black lives.
In spring 2017, Hardeman published another editorial in the Journal of the American Medical Association with Kozhimannil and Medina encouraging health systems to zero in on inequities created by racism. “We need to recognize why race was constructed as a social category and understand how it has shaped health care and policies,” says Hardeman.
To turn research into practice, she’s developing interventions for first-year medical students to teach them about the history of structural racism with Dr. Brooke Cunningham, assistant professor in the University of Minnesota Department of Family Medicine and Community Health. “We’re not only teaching why these inequities exist, but teaching these future doctors how to talk with their patients about how their health outcomes might be a result of structural racism,” says Hardeman.
She has also recently been involved in a training at the University of Minnesota Medical Center attended by all OBGYNs, residents, and midwives about how structural racism has an impact on birth outcomes. “Some of the people in the room had never thought about structural racism before or, if they had, they didn’t relate it to birth outcomes,” Hardeman says.
“Awareness is the first step, and it’s a huge step,” she says. “If my work helps anyone become aware of these issues, then I’ve made a difference.”
Listen to a related podcast interview with Rachel Hardeman, produced by StoneArch Creative in Minneapolis.