Joseline Haizel-Cobbina
MPH, Public Health Administration & Policy
Co-Authors:
Helen Parsons, Logan Spector, Christopher Moertel
Advisor:
Dr. Helen Parsons
Educational Objectives:
Describe how race impacts treatment outcomes of pediatric brain and CNS tumors in the United States after accounting for SES.
Keywords:
Pediatric Cancer, Racial disparities
Abstract
Background: Despite improvements in survival for pediatric cancers, treatment disparities remain for racial/ethnic minorities compared to non-Hispanic whites; however, the impact of race/ethnicity on outcomes for pediatric brain and central nervous system (CNS) tumors are not well-known.
Methods: We included children aged 0 – 19 years diagnosed with primary, malignant brain and CNS tumors between 2000 – 2015 in the Surveillance, Epidemiology and End Results Program. We used Chi-square tests to assess sociodemographic and cancer characteristics by race/ethnicity (non-Hispanic Whites, non-Hispanic Blacks, Hispanics and other racial groups). We then used Kaplan–Meier curves and Cox proportional hazards models to examine differences in 10-year survival by race/ethnicity, adjusting for socio-demographics, cancer and treatment characteristics.
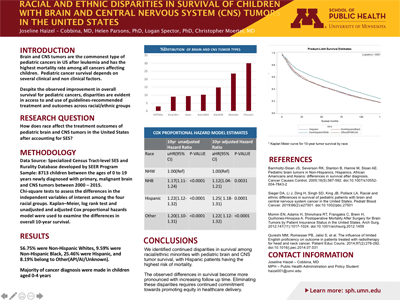
Results: Among 8,713 children with brain and CNS tumors, 56.75% were non-Hispanic White, 9.59% non-Hispanic Black, 25.46% Hispanic, and 8.19% were from other racial/ethnic groups. Median unadjusted survival for all pediatric brain tumors was 53 months, but varied significantly by race/ethnicity (median survival: 62 months for Non-Hispanic whites, 41 months for Non-Hispanic blacks, and 40 months for Hispanics/Other race/ethnicities). Adjusting for socio-demographics, cancer and treatment characteristics, minority racial groups continued to have significantly higher hazard of death than Non-Hispanic whites; Hispanic [aHR 1.25(1.18- 1.31)]; Non-Hispanic black [aHR 1.12(1.04-1.21)]; Other [aHR 1.22(1.12- 1.32)]. Results were consistent when stratified by tumor histology.
Discussion: We identified continued disparities in survival among racial/ethnic minorities with pediatric brain and CNS tumor survival, with Hispanic patients having the highest risk of mortality. Eliminating these disparities requires continued commitment towards promoting equity in healthcare delivery.
View Presentation (PPSX)
