Manami Bhattacharya
PhD, Health Services Research, Policy & Administration
Recipient of the Student Public Health Opioid Research prize, awarded by the SPH Alumni Society.
Co-Authors:
Erin T. Carey, Kristin Moore, Lauren D. Schiff, Michelle Louie; Paula D. Strassle
Advisor:
Dr. Donna McAlpine
Educational Objectives:
Assess whether preoperative depression affects women’s risk of persistent opioid use after hysterectomy.
Keywords:
Opioid use, Women’s Health
Abstract
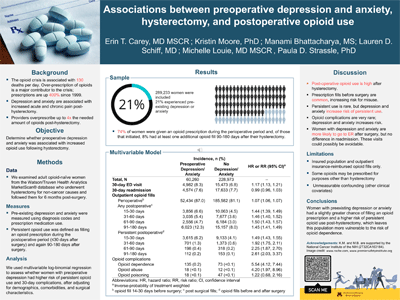
Objective: Preoperative depression has been linked to adverse outcomes following hysterectomy, including increased acute and chronic postoperative pain. The goal of this study was to determine whether preoperative depression was associated with increased opioid use following hysterectomy.
Methods: We examined 383,243 opioid-naïve women from the Watson/Truven Health Analytics MarketScan® database who underwent hysterectomy for non-cancer causes and followed them for 6 months post-surgery. We used multivariable log-binomial regression to assess whether women with preoperative depression had higher risk of persistent opioid use and 30-day complications, after adjusting for demographics, comorbidities, and surgical characteristics. Persistent opioid use was defined as filling an opioid prescription during the postoperative period (≤30 days after surgery) and again 90-180 days after surgery.
Results: The prevalence of pre-surgical depression was 20% (n=75,230). 74% of women were given an opioid prescription during the perioperative period and, of those that initiated, 8% had at least one additional opioid fill 90-180 days after their hysterectomy. In multivariable analyses, women with depression were 8% more likely to get an initial opioid fill (RR 1.08, 9%%CI 1.07, 1.08) and were 43% more likely to have persistent opioid use (RR 1.43, 95% CI 1.39, 1.47). Women with depression were also slightly more likely to have any type of surgical complication (RR 1.04, 95% CI 1.03, 1.06).
Conclusion: Women with preexisting depression had a slightly greater chance of filling an opioid prescription and a higher risk of persistent opioid use post-hysterectomy, which leaves this population more vulnerable to the risk of opioid dependence.
Support
Manami Bhattacharya Kristin Moore are supported by grant T32CA163184 from the National Cancer Institute (NCI) (PI: Michele Allen)
View Poster (PDF)
